What to Expect on
Your First Oral
Hygiene Visit
What to Expect on
Your First Oral
Hygiene Visit
During your first oral hygiene visit, you can expect a comprehensive range of services which promote your oral health.
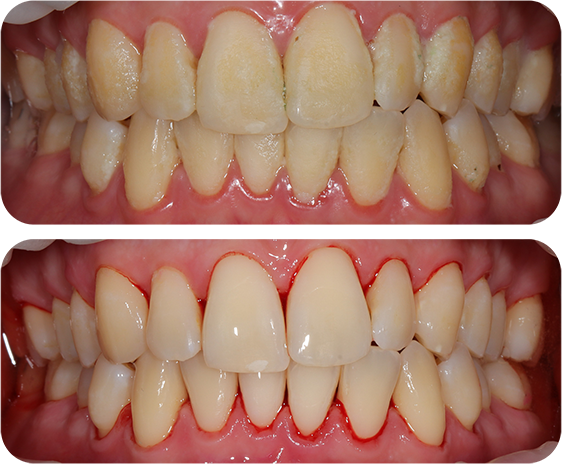
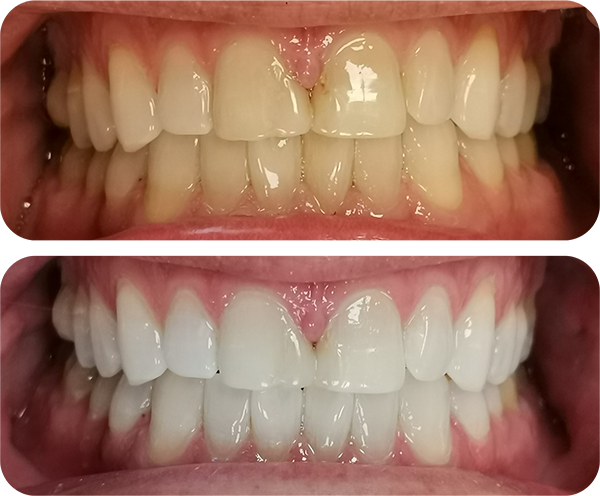
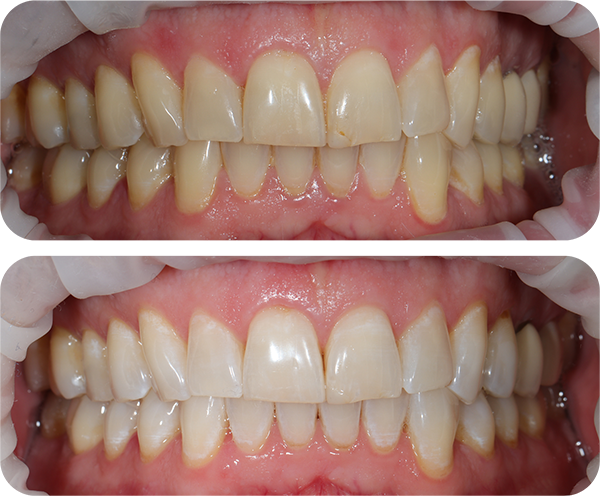
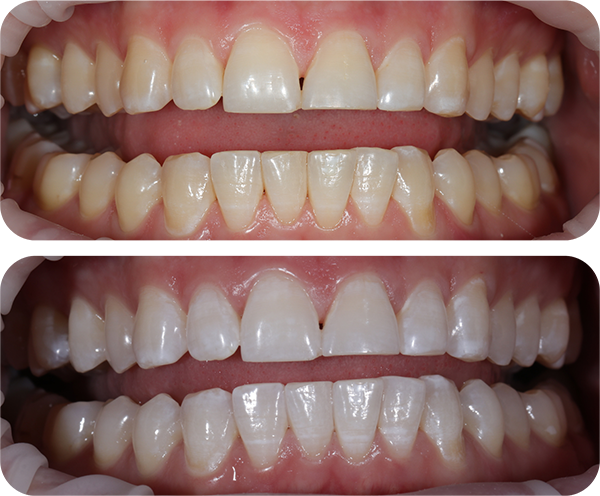
Our highly skilled oral hygienist will perform a professional EMS scale and polish to eliminate plaque and calculus, which are significant contributors to gum disease, dental decay, and tooth loss.
In addition, topical treatments like fluoride may be applied to reduce sensitivity and fortify your teeth against decay.
You'll receive valuable feedback on the effectiveness of your current oral hygiene routine, along with tailored suggestions on products and techniques that suit your individual needs.
To ensure a thorough assessment, our oral hygienist will conduct a check-up to detect any cavities, gum disease, or signs of oral cancer. X-rays may be taken to provide a more detailed evaluation.
Moreover, your visit provides an opportunity to discuss various topics with our knowledgeable oral hygienist. We can address tooth whitening, fissure sealant, orthodontic alignment, bruxism, occlusal guards, mouth guards, and diet advice. There’s no such thing as a stupid question.
Swipe
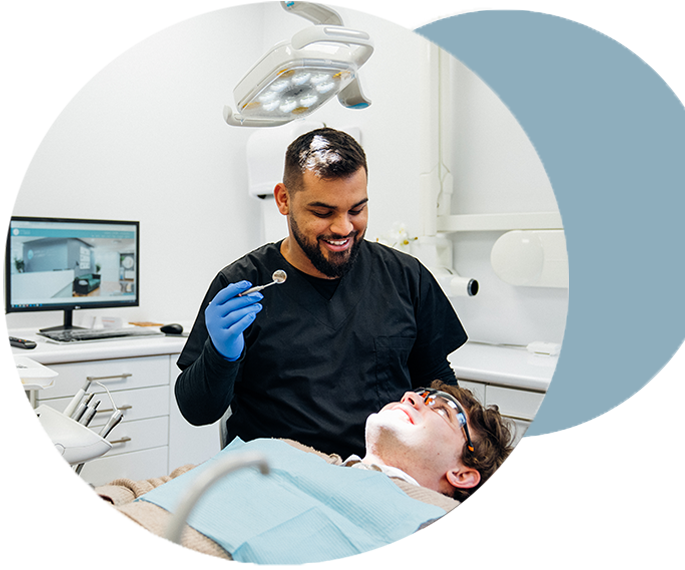
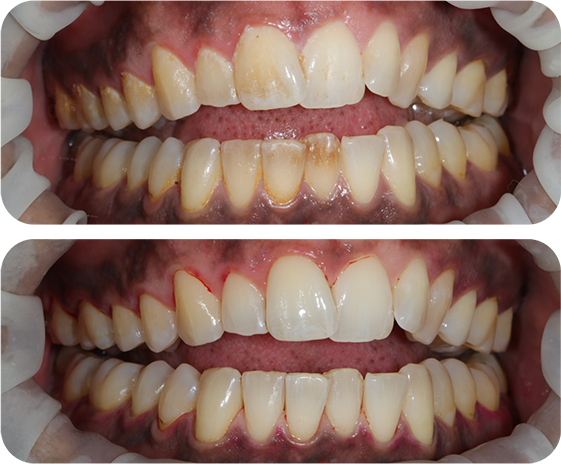
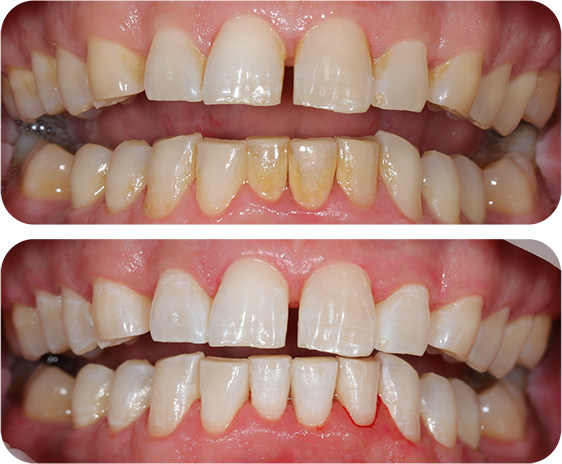
During your first oral hygiene visit, you can expect a comprehensive range of services which promote your oral health.
Our highly skilled oral hygienist will perform a professional EMS scale and polish to eliminate plaque and calculus, which are significant contributors to gum disease, dental decay, and tooth loss.
In addition, topical treatments like fluoride may be applied to reduce sensitivity and fortify your teeth against decay.
You'll receive valuable feedback on the effectiveness of your current oral hygiene routine, along with tailored suggestions on products and techniques that suit your individual needs.
To ensure a thorough assessment, our oral hygienist will conduct a check-up to detect any cavities, gum disease, or signs of oral cancer. X-rays may be taken to provide a more detailed evaluation.
Oral Hygiene for Every Age Group
We believe in providing exceptional oral care to patients of all ages. Our compassionate team is dedicated to delivering personalised treatments and education, ensuring that each generation receives the necessary attention and care to maintain healthy smiles for a lifetime.
Swipe
Paediatric:
Our dental team is experienced in paediatric dentistry, ensuring a positive and fun dental experience for children. We focus on preventive measures, education, and early intervention to promote excellent oral health habits from an early age.
General and Cosmetic:
Our comprehensive services for adults include regular check-ups, cleanings, whitenings and more – enhancing smiles and boosting self-confidence.
Frequently asked questions
Swipe
Tap to reveal
How often should I visit the dentist for a check-up and cleaning?
It is generally recommended to visit the dentist for a check-up and cleaning every six months. Regular visits help detect dental issues early and ensure proper oral hygiene maintenance.
How can I improve my at-home oral hygiene routine?
To enhance your at-home oral hygiene routine, brush your teeth at least twice a day with fluoride toothpaste, floss daily, and use mouthwash. Additionally, replace your toothbrush every three to four months and maintain a balanced diet.
Is teeth whitening safe?
Yes, teeth whitening is safe when performed under professional supervision. Our dental team utilises proven whitening techniques and ensures that the treatment is tailored to your specific needs, minimising any potential risks or discomfort.
What are the benefits of professional teeth cleanings?
Professional teeth cleanings remove plaque, tartar, and surface stains that cannot be eliminated through regular brushing. These cleanings help prevent gum disease, tooth decay, and maintain a fresh and healthy smile.
What can I do about bad breath?
Persistent bad breath may be a sign of an underlying oral health issue. Regular brushing, flossing, and tongue cleaning can help reduce bad breath. If the problem persists, it is recommended to consult with our dental team to identify and address the underlying cause.
Are electric toothbrushes more effective than manual ones?
Electric toothbrushes can be more effective at removing plaque and reducing gum inflammation when used correctly. However, manual toothbrushes can also be effective with proper brushing technique and consistency.
What is the best way to prevent gum disease?
Preventing gum disease involves a combination of good oral hygiene practices. This includes regular brushing and flossing, routine dental check-ups, a balanced diet, avoiding tobacco use, and managing any underlying health conditions that may contribute to gum disease.
How can I manage dental anxiety?
Dental anxiety is common, and our team is experienced in helping patients feel comfortable and relaxed. We communicate openly with patients and provide a supportive and calming environment to alleviate dental anxiety.
Does insurance cover oral hygiene treatments?
Dental insurance coverage varies depending on the specific insurance plan. We are a private practice that does not deal directly with medical aids, however, you are able to submit your claim privately.