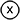What are Dental Implants
Dental implants are the closest you can get to healthy, natural teeth. They allow you to live the way you want to – confidently eating, smiling, laughing, talking, kissing and enjoying all of your everyday activities without worrying about your teeth.
Think of dental implants as artficial tooth roots, similar in shape to screws. When dental implants are placed in your jawbone (A), they bond with your natural bone. They become a sturdy base for supporting one or more artificial teeth, called crowns.




The Difference
Working with a Periodontal Specialists group, we provide specialist implant treatment using the latest technology. Our practitioners are recognised members of the International Team of Implantology and The Implant and Aesthetic Academy.
click to find the difference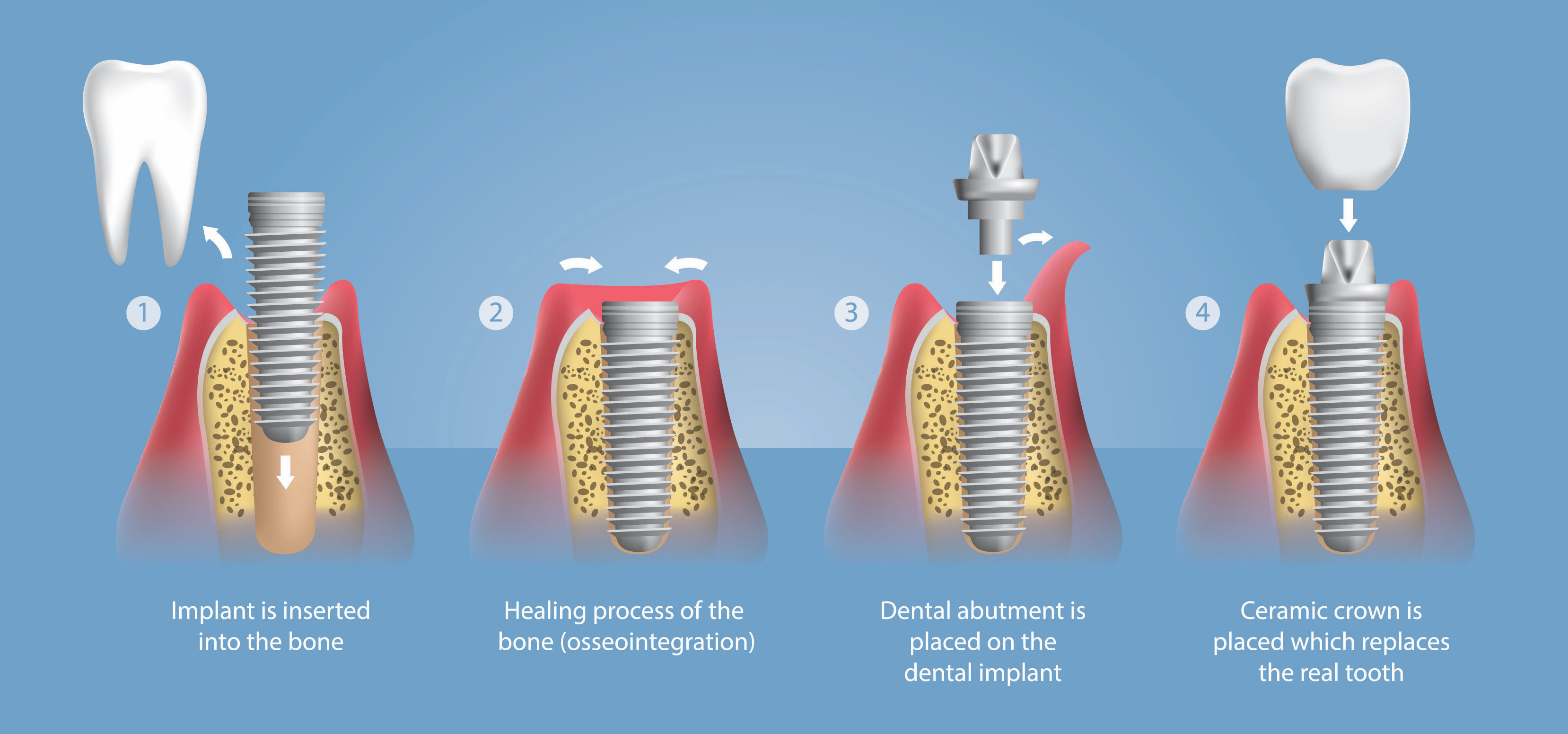
What to expect
After a thoroughly examine of your mouth, including taking Digital X-rays and 3D images, our qualified dentist will discuss your various implant options and develop a plan for your implant surgery. The Dental implant placement treatment usually involves the following steps:
- At your next scheduled appointment, one of our specialists at Cape Periodontal Services will place the dental implant in your jawbone where your tooth is missing. Although each patient’s experience is unique, most people find they experience less pain and discomfort than they expect, and typically return to work the next day. Local anaesthesia or IV sedation can be used to keep you comfortable, depending on the procedure. Post-implant surgery discomfort is similar to that of any other dental surgery. It may include swelling, bruising, minor bleeding and/or pain, but most patients usually manage any pain with overthe-counter medications.
- As you heal, your implant and jawbone will grow together in a process called osseointegration (os-e-o-in-tuh-GRAY-shun), forming a strong, long-lasting foundation for your replacement teeth. During this healing process, which can take up to a few months, you go on with your normal life. You will be on a soft food diet for the first few weeks to make sure your implants heal properly. In some cases, your implant dentist may also be able to place temporary teeth during this period, if you choose.
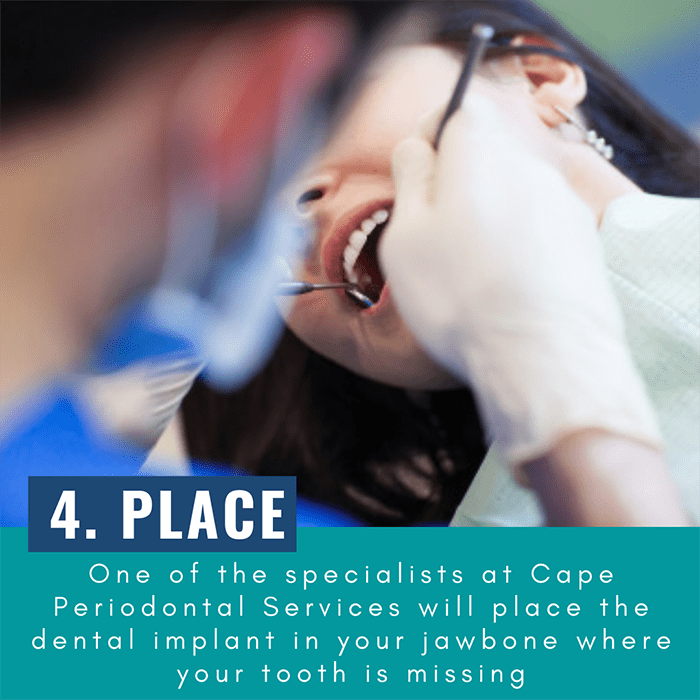
- After your gums heal, we will take an impressions of your mouth and remaining teeth to custom-make your artificial teeth.
- These teeth – which can be an individual crown, implant-supported bridge or dentures containing multiple replacement teeth – will be attached to the abutment. Although they don’t decay, your new teeth will need the same routine care, checkups and cleanings as your natural teeth.
Depending on the number and type of implants and replacement teeth you receive, the entire process can take three to nine months. After your dental implant placement is finished, we will do periodic follow-up check-ups, just as you do regularly.